“Medicine is for the patient, not for the profits.”
--George W. Merck
About a decade ago at a life sciences industry conference I attended, the main topic of one presentation was the need to focus directly on end consumers – the patients and trial participants that are a critical part of research and development. There was silence in the room. Most of the audience agreed that their organizations were not planning to focus on direct discussions with consumers anytime in near future. All I can say is what a difference 10 years makes! Today, for the life sciences industry, success is tied to patient care. In the current healthcare environment, patient care may means collaborating across the healthcare ecosystem and coordinating care through digital technologies, like mobile apps, wearables, and self-service portals. To get it right, organizations need to structure every aspect of their operations around the question, “How will this help our patient?” In other words, life sciences organizations are realizing they need to be patient-centric. So, what changed?
Learning to re-focus on the patient
For many years, physician relationships were the only relationships that mattered. Educate physicians on the newest drug. Get them to write scripts. Boost the bottom line. Though patients were the end-users, organizations focused their efforts on building relationships with the physicians who wrote the prescriptions.
Then a number of issues changed the conversation. Physicians’ offices were saturated with pharma sales reps. The selection of pharmaceuticals available on the market grew, as did pricing options. Payers, pressured to contain costs, began asking life sciences orgs, “Why should I cover your drug? What value-added services are you offering?” And direct-to-consumer pharmaceutical advertising steadily increased.
The industry realized the importance of patient choice and began building out systems to inform and connect with patients. But like many complex businesses, the operational structures of life sciences organizations were, and still are, siloed. That’s because, when well-intentioned business leaders start to think about the patient at the center, they invariably start with a brand, a channel, or a department and neglect to evaluate all the ways in which a patient interacts with their organization. This leads to disconnected systems and data, fragmented patient experiences, and operational siloes – making it difficult for organizations to engage with patients in one, unified, coordinated voice from the very first interaction to the last.
The 7 pillars of patient engagement
The traditional approach to patient engagement is disconnected, siloed, and not working. That’s why the most common question I hear from life sciences organizations today is how they can place the patient at the center of their operations. Patient-centricity is affected by internal systems (e.g., safety, sales, marketing, clinical trials, laboratory information management, medical affairs, medical science) and external systems (e.g., health information exchanges, electronic health records, electronic clinical data, provider care management, Star ratings, IoT devices, SPOR/FDA). To be truly patient-centric, life sciences organizations need to think holistically about the patient’s “end-to-end” journey across all systems, and how to keep the patient and their unique needs at the center of it all.
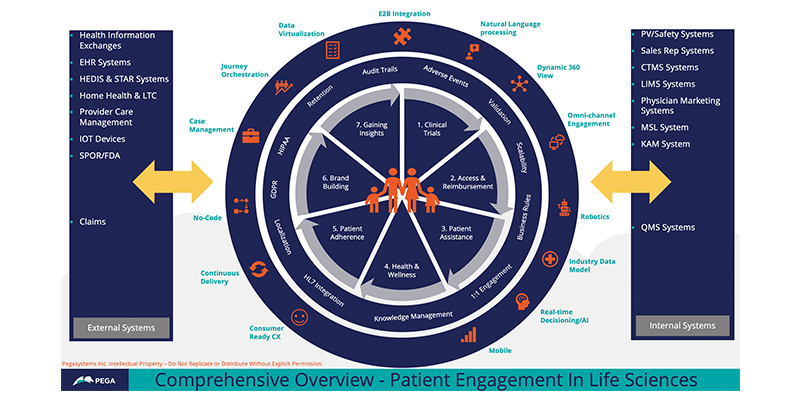
To be truly patient-centric, life sciences organizations need to think holistically about the patient’s “end-to-end” journey across all systems.
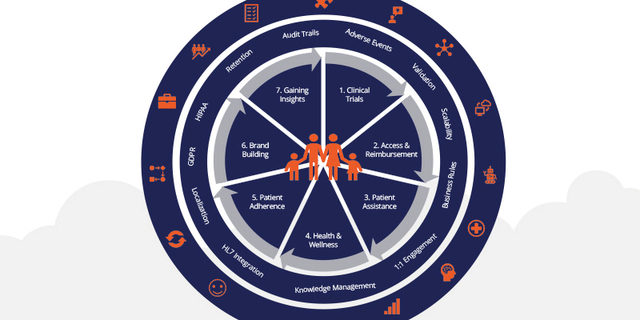
How can your organization be more patient-centric? Look at all of your activities from a high level. The following business areas affect patients the most, so think of these as your foundational elements for patient engagement:
- Clinical Trials: Includes protocol development; participant identification, recruitment, and retention; and adverse event management. The ultimate goal is to bring new therapies to market, and patient interaction is essential at all phases. Patient-centricity in clinical trials means never forgetting that the participants are people with their own unique lives and needs. Engage with empathy in every interaction and make sure requests are reasonable and practical from the patient’s point of view.
- Access & Reimbursement: Includes recruitment/enrollment; benefits verification; prior authorization; and co-pay assistance. If a patient is written a prescription, they need to be able to fill it. Organizations may need to provide support for benefits verification through the payer, prior authorizations, step therapies, and co-pay issues.
- Patient Assistance: Includes enrollment; benefits verification; and assistance disbursement. If, for some reason, a patient does not have access to a therapy, look for other ways to support them. This could be through a charitable arm or foundation as well as third-party organizations or programs that will cover the cost of the treatment or provide general help.
- Health & Wellness: Includes condition education; health coaching; wellness programs; and patient group advocacy. Take an active role in helping to educate patients on their disease states and how to stay healthy. Create internal and external patient advocacy groups to incorporate the voice of the consumer who has lived the experience.
- Patient Adherence: Includes recruitment/enrollment; clinical support; social determinants of heal (SDOH) support; retention; and personalized medicine. If your patient is on a prescribed, long-term therapy (e.g., for hypertension), think about how you can best support them to follow the instructions for that therapy to stay on it and stay healthy. Care management programs are designed to support such needs.
- Brand Building: Includes coupons/vouchers; direct-to-consumer marketing; patient advocacy; recall management; and medical information. Ultimately, building your brand is really helping people understand who your organization is and how you help people. Patients want to know that you are committed to doing the right things for the right reasons.
- Gaining Insights: Includes payer collaboration; Real World Evidence support; and any activity connected to improving patient outcomes. Insight is really a constant, ongoing, cyclic process, fed by data from all of the other activities above.
How to determine if your systems are driving patient-centricity
To determine your organization’s ability to be patient-centric, assess your systems by asking these questions: Are you able to operationalize the data from all of your patient engagement channels, or is your data sitting unused in a warehouse or data lake? Are your departments/workgroups engaging with patients individually in an uncoordinated way? Do you have a central way to start orchestrating patient-related actions across your entire organization, one outcome-based microjourney at a time? Can you leverage your existing investments in these pillars and still make it act like one system for patients? What can you do to expedite patient-centricity across all processes?
As life sciences organizations, your work is critical to patient health, and positive patient outcomes are essential for your success. Engage with your patients on an empathetic and personal level. Create an environment where they feel confident that, no matter who or how many of your staff they engage with on any channel, they are supported by one team dedicated to their best health.
Learn more:
- Download our eBook to understand why healthcare engagement should be personalized prioritized and preemptive.
- Read more from Jitesh on personalizing wellness programs and understanding how GDPR is related to health data and consent.
- Discover how Pega for Healthcare & Life Sciences is personalizing patient engagement for better health outcomes.